Introduction
A distal radius fracture is a fracture of the radius bone that occurs at the level of the wrist. This fracture is the most common fracture of the upper extremity, and one of the most common fractures encountered by orthopedists. Due to their common nature, distal radius fractures are colloquially called “wrist fractures,” even though they do not make up the entirety of fractures of the wrist. In this article we will discuss some general information pertaining to distal radius fractures.
Anatomy
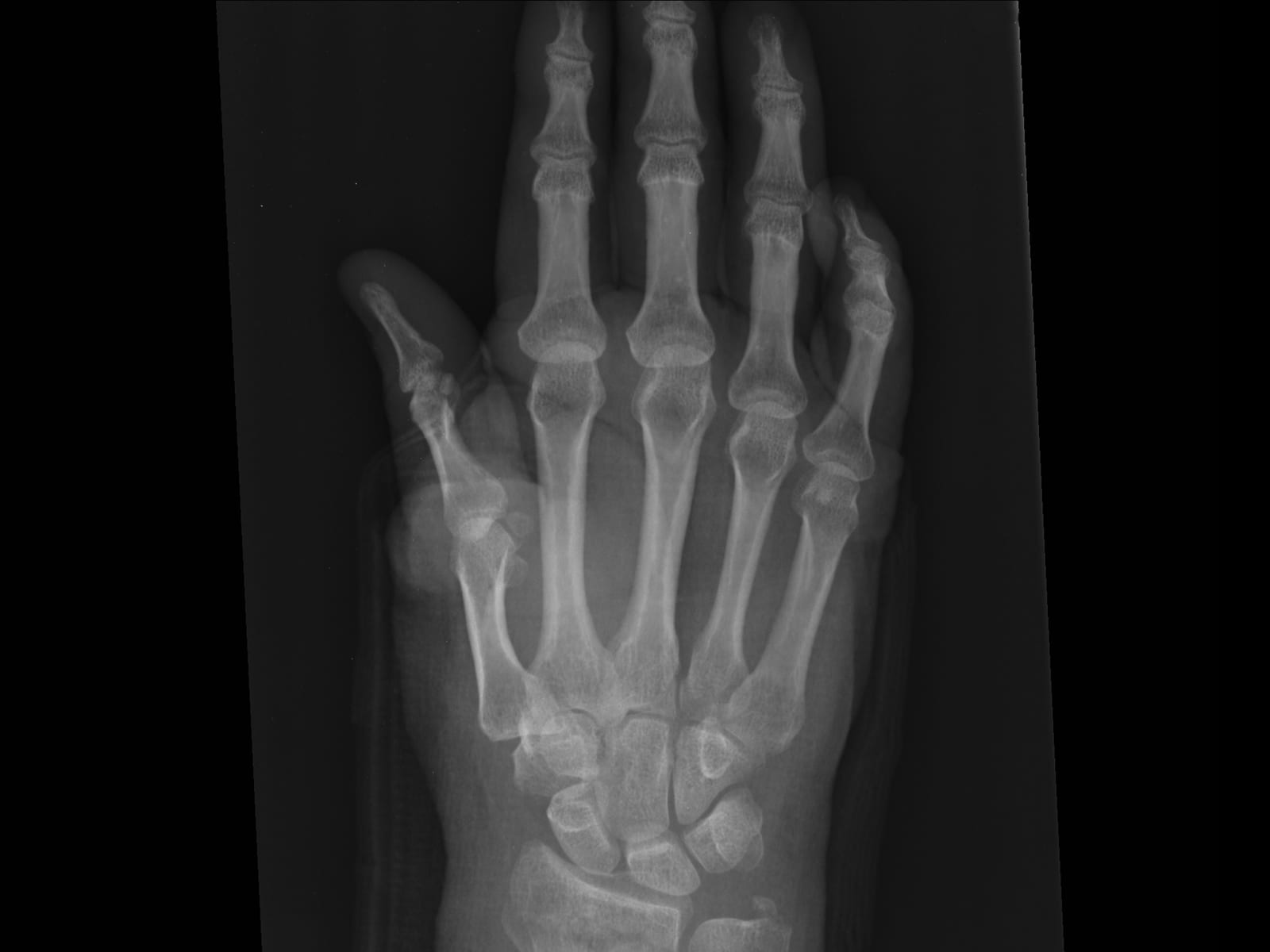
The wrist is a complex structure made up of several bones including the radius, the ulna, and several carpal bones within the hand. The scaphoid and lunate are two carpal bones that, along with the radius, form the radiocarpal joint. This is a modified ball-and-socket joint that permits motion in several directions.
The radius and ulna are also the two bones of the forearm. These two bones form joints with each other at the elbow and at the wrist, allowing rotation of the forearm. At the level of the wrist, this joint is called the distal radioulnar joint (DRUJ).
In a distal radius fracture, the radius is broken near the wrist in an area of less dense bone called the metaphysis. If a fracture is extra-articular, this means the fracture line does not enter into the joint. When a fracture is intra-articular, the fracture enters into the joint.
Sometimes the ulna bone can also be fractured along with the radius. Also, some wrist fractures can affect the stability of the DRUJ. As a result, fractures of the wrist can affect not only the wrist joint, but also the forearm.
Mechanism of injury
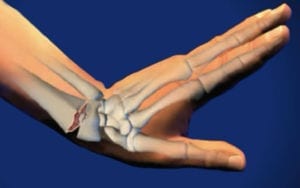
Distal radius fractures result when the energy transmitted to the wrist is sufficient to overcome the innate strength of the bone. The bone is naturally weaker and spongier in the metaphysis of the distal radius, making it prone to fracture with trauma.
The most common mechanism of injury is a fall on the outstretched hand. Most often, the wrist is in an extended position when the hand breaks the fall, resulting in a force that fractures and collapses the back side of the distal radius and distracts the palm side. The fracture causes the radius bone to angulate backwards. This is the most common fracture pattern, and is called a Colles fracture, named after a 19th century Irish surgeon. Depending on the particular position of the wrist and direction of the forces, many different fracture patterns may occur.
Symptoms
A distal radius fracture can present with several symptoms. Common symptoms include pain, swelling, bruising, numbness, and a visible deformity. The deformity most commonly encountered is the “dinner fork” deformity caused by Colles type fractures. The angulation and displacement of the fracture give a humped appearance to the wrist. This typical deformity was, in fact, how Dr. Colles came to identify the fractures.
The presence of these symptoms after trauma highly suggest the need for further evaluation by a doctor in the emergency setting and for X-rays to further understand the injury. One additional finding that can drastically change management is when the fracture communicates with the outside world through a break in the skin. Termed an “open fracture,” these are severe injuries that need to be treated surgically on an emergent basis.
Imaging
Initial imaging studies consist of X-rays. These are critical to help understand the injury. They provide information as to how severe the fracture is, how displaced the fracture is, whether the fracture enters the joint, the quality of the bone, and many other things. X-rays help tremendously to guide future treatment.
On occasion, additional advanced imaging studies such as a CT scan will be obtained. These are most useful to the surgeon that is planning on operative treatment.
Initial Management
Fractures that are widely displaced should have a reduction maneuver performed in the emergency setting, followed by splinting of the injury. A reduction maneuver is the application of force to a fracture in an attempt to improve the alignment of the fracture. Reducing the fracture helps to improve pain, limit further soft tissue injury caused by fracture displacement, and decrease pressure on nerves or blood vessels near the fracture. A successful reduction may also help to avoid surgery. A splint applied to the bone will help support the reduction, protect the wrist from further injury, and decrease pain.
Surgery
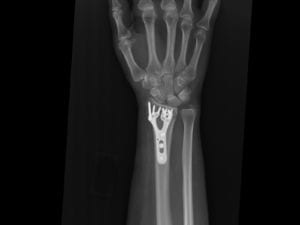
In deciding whether a patient is better off treated with or without surgery, the surgeon will consider characteristics of both the fracture and the patient. In the appropriate patient, when xrays show that alignment is inadequate, surgery is recommended. The goal of surgery is to restore acceptable alignment while providing the stability to allow early motion and rehabilitation. Hardware, typically a variety of plates and screws or pins, are inserted into the bone to hold the proper alignment until the bone heals.
After surgery, the surgeon decides the appropriate time to start range of motion to optimize the patient’s recovery. Typically range of motion exercises are started after 1-2 weeks of full time immobilization, and splinting may continue for about 4-6 weeks. Fractures usually heal within 6 weeks, but the recovery from a wrist fracture can often extend longer, continuing for several months and sometimes past the first year.
Conservative Management
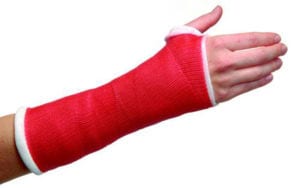
In general, if fractures are minimally displaced or if alignment on x-rays after reduction is felt to be adequate, the fracture can be treated without surgery. Conservative treatment then proceeds with immobilization, typically in a cast. Depending on the fracture, return visits for follow up X-rays spaced 1-2 weeks apart may be necessary to ensure that the fracture alignment is maintained during immobilization. A fracture that significantly displaces with cast treatment may be better treated with surgery. The total duration of immobilization depends on the severity of the fracture and healing taken place, but usually lasts for 4-6 weeks. A splint can then be used intermittently as motion is regained.
Goals of treatment
The ultimate goals of treating a distal radius fracture are:
- Healing of the fracture in an acceptable alignment
- Preservation of painless wrist and forearm range of motion to allow positioning of a well functioning hand for daily activities
Because of the importance of hand function, patients are encouraged early on while in a splint or cast to maintain full range of motion of the fingers. Oftentimes, patients will benefit from occupational therapy after surgery or conservative treatment of distal radius fractures. The goal of therapy is to manage pain and allow the patient to regain motion, strength, and function. Most patients resume good function by 3 months, but on occasion recovery may take longer.
Have you injured your wrist? Request your appointment here.