Introduction to Thumb CMC Osteoarthritis
Pain that is present around the base of the thumb and made worse with use of the hand is most often caused by osteoarthritis of the thumb carpometacarpal (CMC) joint. The thumb CMC joint is the joint most likely to develop painful arthritis in the human body. More than one out of five people older than 40 are affected. When severe, the pain will impair normal hand function. Thumb CMC joint osteoarthritis is one of the most common conditions seen by a hand surgeon. Although it is very common, many people are unaware that there are several treatment options to address pain and improve their quality of life.
Anatomy
The thumb is one of man’s most important anatomic features. It plays a vital role in most hand functions through a combination of flexibility and strength.
Whereas the other joints of the thumb are shaped like hinges that flex and extend the joints, the thumb CMC joint has a saddle-like shape that allows the thumb to move in various planes. This provides the thumb the flexibility to position itself in space so that it can interact with the world and its objects. The large thumb muscles can apply forces delicate enough for a precision pinch or strong enough for a power grip. Given its importance, it should be no surprise that without the thumb, the hand loses about 50% of its function.
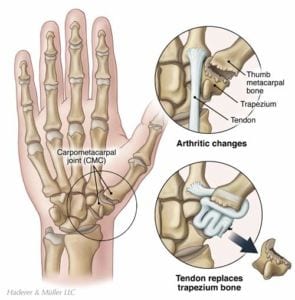
Although the thumb CMC joint seems elegantly designed, the freedom of mobility and tremendous demands placed on the thumb predispose it to developing osteoarthritis. The laxity essential for allowing a wide range of motion often translates into instability, which leads to premature cartilage wear. In addition the biomechanical design of the thumb multiplies the muscle forces crossing the joint by a factor of 12, meaning that the joint cartilage is exposed to large forces. As a result, the thumb CMC joint is one of the body’s joints most susceptible to osteoarthritis.
Symptoms
Most patients present with complaints of pain, aching, or burning at the base of the thumb. The pain is often vague or difficult to pinpoint, and as such may be interpreted as arising from the hand, thumb, or wrist. Use of the hand typically makes the pain worse. Activities that are particularly painful include:
-
-
- forceful pinching (such as when holding dishes, turning a key, or pulling up a pair of pants)
- forceful grip (such as opening a jar).
- extremes of motion (such as reaching across to the small finger or spreading the hand open)
-
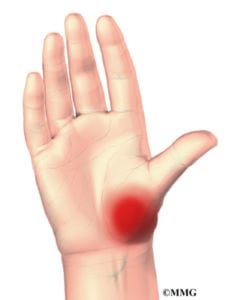
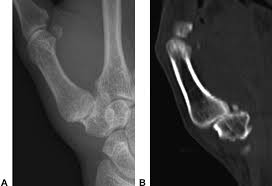
When the condition is severe, even light activities can be painful. On examination, there is typically tenderness at the CMC joint or pain when the joint is forcefully compressed. Xrays show findings typical of osteoarthritis, including loss of cartilage, bone spurs, and loose bodies.
Treatment
Nonoperative
When I see patients with thumb arthritis, I feel it is important to lay out the goals of care: reduction of pain and improvement of function. Patients should embark on a trial of nonoperative treatment because many people can improve without surgery. Activity modification, use of assistive devices, and splinting of the thumb CMC joint are a good place to start.
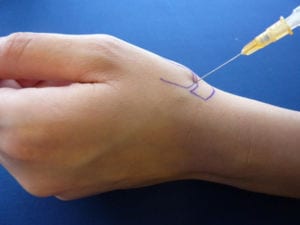
Nonsteroidal anti-inflammatories or acetaminophen can also help improve pain. A steroid injection into the joint may provide temporary relief. These efforts may ultimately help improve pain and function. In some they may delay or eliminate the need for surgery.
Surgery
When nonoperative measures have failed to adequately improve the condition, surgery is recommended. Many patients are unaware that surgery can, in fact, help their condition. There are several different types of surgeries that reliably improve pain and function. The most common procedure involves the removal of the trapezium (one of the bones forming the CMC joint), reconstruction of the ligaments that stabilize the thumb, and filling of the space left by trapezium removal with a tendon spacer. In young laborers, a fusion of the joint is an option. Another type of surgery replaces the joint surfaces with artificial implants, as in hip or knee joint replacements. In patients with painful early arthritis, procedures that preserve the trapezium, such as a scope and cleanup of the joint, can be performed. The surgeon will decide which operation is best for a patient’s particular case.
Recovery
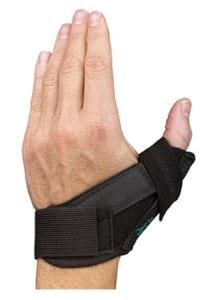
After surgery patients require a short period of protective splinting, usually 4-6 weeks, and most benefit from hand therapy to regain motion and strength. Depending on their job demands, a patient may return to work within 2-10 weeks. A durable improvement in pain, strength, and function can reliably be achieved in over 90% of patients, and there is a high satisfaction rate after surgery.
Do you need treatment for your thumb pain? Let’s get you treated. Request your appointment here.